NCS Journal Club Round-Up #NCSTJC: October 2023
Published on: February 02, 2024
 Moderator: @theABofPharmaC
Moderator: @theABofPharmaC
Authors: @brainicudoc, @lakim22
Link to Twitter Thread: https://twitter.com/neurocritical/status/1711743402834837557
The October Neurocritical Care Society Twitter Journal Club featured a discussion on the article “Safety and Efficacy of Ketamine Without Intubation in the Management of Refractory Seizures: A Case Series” by Lauren Kimmons et al. The series had a goal of describing the efficacy and safety of the use of ketamine in non-intubated patients with refractory seizures. The authors retrospectively reviewed a cohort of patients in whom ketamine infusion was initiated for refractory seizures without intubation. The study included 28 patients who were divided into groups of ketamine-responders and non-responders.
A broad discussion on the article was held Twitter (X) for the #NCSTJC, and we review the topics and opinions expressed by participants below.

Discussion began with a poll prompting participants to indicate their own practice in the use of ketamine. @salia_farrokh, @caseyalbin, and @tchaaban1, reported all having used ketamine, primarily in intubated patients. @tchaaban1 mentioned their practice of using ketamine in patients who failed a benzodiazepine infusion. Out of 128 votes, 53.1% reported a similar practice, exclusively using ketamine in intubated patients. However, 25.8% voted that they have used ketamine in refractory status epilepticus (RSE) and in non-intubated patients. The remaining 20% have not used ketamine at all. @brainicudoc underscored the importance of early initiation of ketamine, particularly in elderly patients, those with high mortality, or patients who are Do Not Intubate (DNI) presenting with RSE.
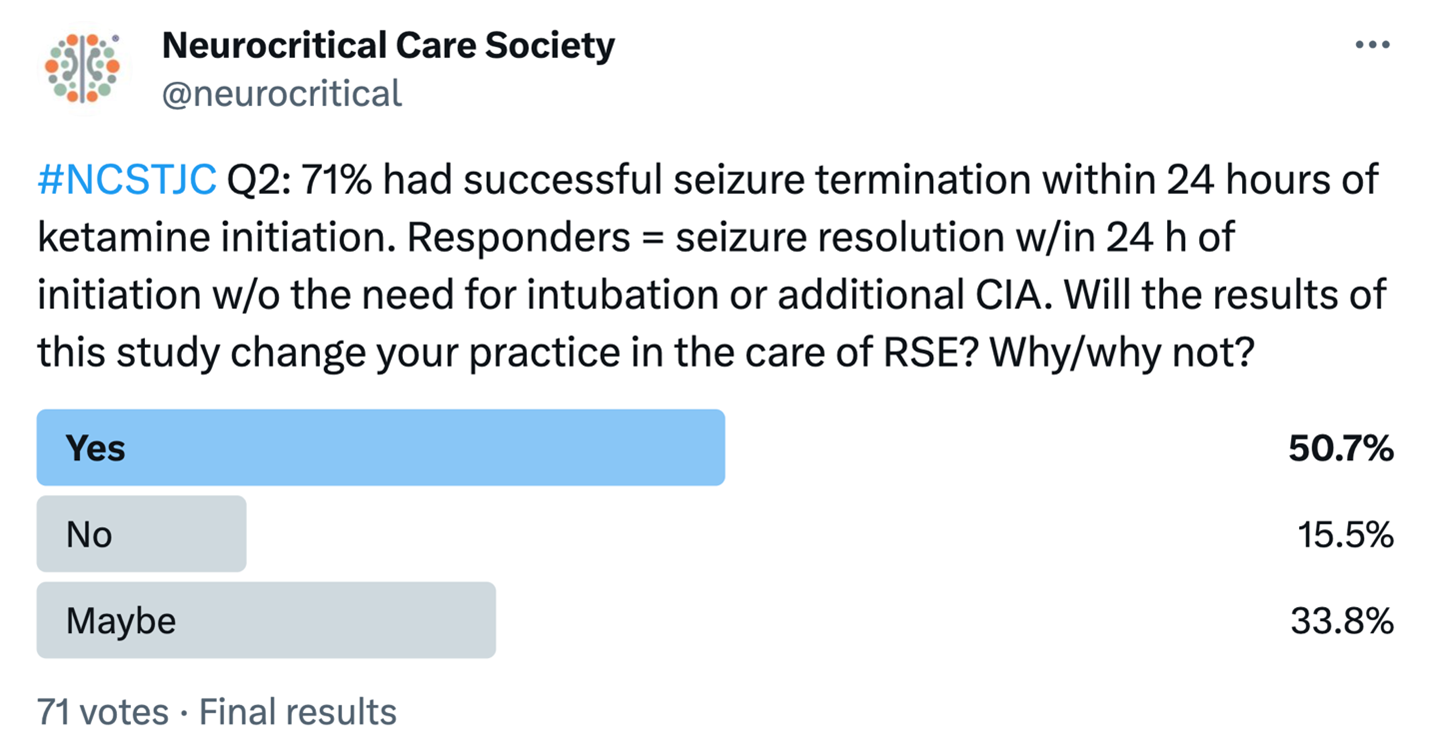
Question 2 featured a poll asking participants if the study changed their perspectives on the use of ketamine. Out of 71 votes, 50% indicated that the article would lead to a change in their practice for refractory status epilepticus (RSE), while 33% expressed a "maybe," and 15% stated that it would not. @tchaaban1 highlighted that most patients had focal seizures, raising questions about the necessity of intubation in these cases and suggesting a lower likelihood of generalized RSE. They emphasized the importance of 24-hour seizure termination but called for additional data on length of stay, neurological outcomes, and mortality. Similar perspectives were shared by @theABofPharmaC and @DrAmir_Saeed.

Question 3 included a lively discussion led by @salia_farrokh, @dionneswor, @NezerSara, @NICUintheD, @brainicudoc, @gdomeni, @j_Equiza. The consensus in the group was to consider using ketamine in refractory status epilepticus (RSE) for patients with a history of epilepsy (53.6%) and a structural seizure etiology in 82.1% (such as intracerebral hemorrhage, stroke, or brain tumor). They collectively leaned towards using ketamine in the context of focal RSE, with a primary goal of avoiding intubation, especially in patients with a Do Not Intubate (DNI) status. The prevailing sentiment was to initiate ketamine earlier in the treatment protocol to prevent the progression to status. @salia_farrokh specifically advocated for using ketamine after benzodiazepines and second-line agents but before barbiturate coma. Additionally, they highlighted the preference for ketamine over propofol to avoid propofol infusion syndrome and to target a different mechanism of action.

In addressing the management strategy for hemodynamic alterations in patients receiving ketamine, @lakim22 and @theABofPharmaC observed that hemodynamic changes are less common or severe when ketamine is used as a solo agent rather than in combination with other anesthetics. They suggested most alterations can be managed with fluids, pressors, or antihypertensives without adjusting the ketamine itself. Instances of bradycardia with bolus doses were noted in the study, with hypotension attributed to combined effects or systemic illness. @brainicudoc underscored the rarity of stopping ketamine treatment, advocating for the addition of low-dose norepinephrine. Additionally, monitoring for side effects such as agitation and occasional use of dexmedetomidine or intermittent long-acting benzodiazepines were discussed. @gdomeni highlighted ketamine's favorable hemodynamic profile, noting the potential benefit of avoiding mechanical ventilation.

In question 5, @theABofPharmaC emphasized the importance of early intervention in neurocritical care, echoing the sentiment that "time is brain." Despite this, the exact timing of treatment escalation after failure of first/second-line agents in RSE remains undefined. @NICUintheD offered some clinical guidance, suggesting the transition to continuous infusion anesthetics approximately 40 minutes after generalized convulsions persist despite adequate benzodiazepine and anti-seizure medication dosing. EEG findings of >10 mins continuous seizure activity after adequate medication dosing also indicated the need for anesthetic treatment.

The Twitter discussion on ketamine use for non-intubated patients with refractory status epilepticus (RSE), featured insights and best practices from multiple participants. @SwarnaRMD highlighted the need for close airway monitoring, noting ketamine's potential to increase secretions in patients with acute brain injury. @NICUintheD recommended restricting ketamine use to the ICU, emphasizing invasive hemodynamic monitoring and prophylactic glycopyrrolate to manage secretions. @KeatonSmetana underscored the importance of monitoring ketamine concentration and watching volume status closely, especially as it can be a limiting factor at higher doses. @Nicole_Davis026 shared her institution's experience with an undiluted ketamine bag, emphasizing careful titration to avoid issues. @brainicudoc stressed the necessity of an ICU setting with experienced providers, tailoring dosing based on patient response, and maintaining a low threshold for intubation if needed.
@tchaaban1 suggested implementing an arbitrary dose cap until more safety data is available, and @lakim22 recommended an ICU setting for EEG, airway management, and hemodynamic monitoring. Additionally, she highlighted the importance of consulting institutional policies, collaborating with pharmacists, and establishing clear communication on monitoring parameters with nursing staff.
***
The October edition of the #NCSTJC included a great discussion of the use of ketamine in both intubated and non-intubated patients with refractory status epilepticus. The online discussion showed some consensus on the topic, such as the early initiation of ketamine, but also addressed safety concerns, such as appropriate dosing and increased secretions. The authors of the study concluded that ketamine can be a safe and effective treatment option that has the potential to reduce morbidity and intubation rates.
Read the full article here: https://link.springer.com/article/10.1007/s12028-023-01811-4